Borderline Personality Disorder (BPD) is a deeply misunderstood mental health condition. Characterized by intense emotional instability, turbulent relationships, and impulsive behaviors, BPD is a serious but treatable condition that affects around 1.6% of the population — though some studies suggest it may be closer to 5.9%.
Classified under the Cluster B personality disorders, BPD typically develops during adolescence or early adulthood and disproportionately affects women, though men are often underdiagnosed. Despite being stigmatized as untreatable, research and lived experiences show otherwise.
Understanding Borderline Personality Disorder
People with BPD often struggle with regulating emotions and maintaining a consistent sense of self. They may experience intense fears of abandonment and rapidly shifting views of themselves and others, making stable relationships challenging.
According to the National Institute of Mental Health (NIMH), BPD involves ongoing patterns of varying moods, self-image, and behavior. These symptoms often result in impulsive actions and problems in relationships.
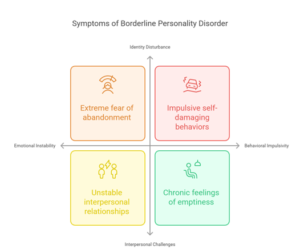
Key Symptoms Include:
- Extreme fear of abandonment
- Unstable or intense interpersonal relationships
- Identity disturbance or poor self-image
- Impulsive, self-damaging behaviors (e.g., substance use, reckless driving)
- Self-injury or suicidal behaviors
- Chronic feelings of emptiness
- Inappropriate or intense anger
- Dissociation or paranoid ideation during stress
For a complete diagnosis, individuals must meet the criteria listed in the DSM-5.
Risk Factors and Causes
While the exact cause of BPD is not fully understood, research suggests that it develops from a combination of genetic, neurological, and environmental factors.
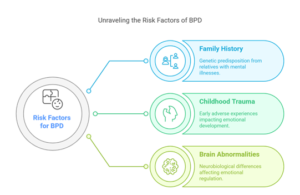
Common Risk Factors:
- Family history of BPD or other mental illnesses
- Childhood trauma such as abuse, neglect, or abandonment (American Psychological Association)
- Brain structure and function abnormalities affecting emotion regulation (Harvard Health Publishing)
Additionally, people with co-occurring conditions like PTSD, anxiety, depression, or eating disorders may be more vulnerable to developing BPD.
Diagnosis and Treatment
Diagnosing BPD requires a thorough psychological evaluation, often using tools such as the Structured Clinical Interview for DSM Disorders (SCID-5-PD).
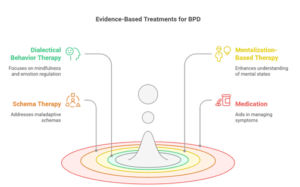
Evidence-Based Treatments:
- Dialectical Behavior Therapy (DBT) – Developed by Dr. Marsha Linehan specifically for BPD, DBT integrates mindfulness, distress tolerance, emotion regulation, and interpersonal effectiveness.
- Mentalization-Based Therapy (MBT) – Helps patients better understand their own and others’ mental states.
- Schema Therapy – Addresses early maladaptive schemas that affect behavior and perception.
- Medication is not a primary treatment but may help manage co-occurring symptoms like anxiety, depression, or mood swings (Mayo Clinic).
Prognosis and Recovery
Contrary to outdated assumptions, people with BPD can and do recover. In fact, research shows that with treatment, 88% of patients experience symptom remission within 10 years (Harvard Review of Psychiatry).
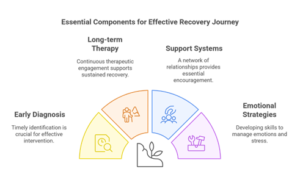
Key Elements of Recovery:
- Early diagnosis and intervention
- Long-term commitment to therapy
- Strong support systems
- Development of emotional regulation and coping strategies
Many individuals report significant improvement by their 30s or 40s, and a growing number of people in BPD recovery now share their stories through blogs, podcasts, and social media—helping to dismantle the stigma.
Breaking the Stigma
Stigma remains one of the biggest barriers to BPD recovery. Misconceptions like “people with BPD are manipulative” or “too difficult to treat” are harmful and untrue. These stereotypes are rooted in misunderstanding and prevent people from getting help.
Efforts by organizations like NAMI (National Alliance on Mental Illness) and mental health advocates are working to change that by promoting education, empathy, and evidence-based treatment.

Conclusion: A Future of Healing
BPD is not a life sentence. While it presents unique challenges, many people go on to live meaningful, connected, and emotionally rich lives. With the right combination of therapy, support, and self-awareness, healing is absolutely possible.
Understanding and compassion are key. Whether you’re living with BPD or supporting someone who is, remember: recovery is real, and you are not alone.

Contact Us or Request an Appointment
Mail us at: support@thebpdcollective.com
Website: www.thebpdcollective.com

Leave a Reply